AIMS Journal, 2021, Vol 33, No 1
To read or download this Journal in a magazine format on ISSUU, please click here

By Alex Smith
Oliver is nearly six months old. Until now, his mother Eileen has been allowed to feed him at home; he is breastfed and so the risks are minimal. Had he been formula fed, she could still have fed him at home but only under regular supervision. This is because Eileen is not a trained infant feeding practitioner, nor is she qualified to recognise the early signs of gastroenteritis and other potential medical issues associated with this higher risk situation. Very soon, Oliver will be prescribed an introductory diet of solid foods by his paediatrician and will join his family and neighbours to take every meal together at their local community eating centre.
It may be difficult to imagine, but things were not always this way. Before the Family Nutrition Report was published, many decades ago now, the majority of families planned, prepared and ate their own food at home, but this came at a dreadful price. A government enquiry found that morbidity and mortality from accidents and illness directly associated with home cooking and eating was unacceptably high and largely avoidable. These direct causes included chip-pan fires, food poisoning, choking, burns and knife injuries. Even greater in its impact, the enquiry found, was the indirect effect of poor nutrition on the rates of illnesses such as diabetes, heart disease, gastrointestinal problems and many cancers. In all, the report found that the costs to the country in terms of the use of precious NHS resources and lost days at work could not be sustained on either economic or ethical grounds. In conclusion, it recommended that all families should have access to free-at-the-point-of-contact eating centres where balanced meals would be available throughout the day, to be enjoyed in the safety of a specially designed environment attended by medical experts trained in nutrition and the Heimlich manoeuvre.
Surprisingly, there was very little resistance to this new policy. Academics believe that this is explained by the growing concern about food poverty and obesity at that time; the steady demise of the family meal; the fact that working practices found more and more children already eating breakfast at school; and the idea of eating out or ordering takeaway becoming much more normal. The thrice daily use of an eating centre situated on every street corner, with no need to take responsibility for shopping, cooking and washing up, was an attractive and welcome prospect for most families. In fact, the scheme was successfully promoted with the government slogan, ‘Don’t do a thing: Eat like a King’, which tapped into the suggestion that the upper classes had always eaten out or employed a professional cook. The report did not specifically ban home cooking and eating, indeed, these things are one’s human right and protected by law, but people are no longer prepared to take unnecessary risks, preferring instead to leave culinary matters to the experts; and safety apart, few people these days would welcome the mess and palaver that home cooking and eating used to entail.
Unfortunately, a lack of funding and under-staffing means that the eating environment is invariably functional, the pace rushed, and the menu limited; you rarely see the same staff twice. These factors were cited in recent research as possible reasons why community eating centres have not seen improved outcomes in the way that was hoped. However, the majority of people are reassured to know that while eating, friendly staff will watch them closely to check that they are chewing and swallowing properly and that gastrointestinal motility meets normal measures. In addition, people value the routine weight, stool and blood tests that check for signs of illness that might otherwise have been missed.
While today, our primal instinct to gather and prepare food is vicariously satisfied by watching programmes such as ‘Call the Chef’, the actual idea of an intimate candlelit meal prepared and eaten at home involves skills that have been lost over succeeding generations and is both indulgent and archaic. The important thing is that everyone gets safely fed. Eileen and Oliver are so lucky to have help at hand!
Whether or not this offers you a utopian or dystopian sense of life on Pathogenia is a personal call, but even in drafting this rather obvious analogy, I almost had myself convinced!
Eating and digestion are normal physiological processes. Almost all physiological processes are entrusted to our good sense to manage safely at home despite the numerous complications that can arise. We are not without expert advice on these matters, but the decision-making is known to be ours, and ours alone. This is because the integrity of the body is enshrined in law; we cannot be forced to eat our greens. We are credited with the ability to recognise and self-treat minor issues in family-preferred ways, and to know or sense when to consult a pharmacist or doctor. Until that point we take an entirely positive or salutogenic approach in taking care of our physiological well-being, and this is widely encouraged. The one exception is the normal physiological process of pregnancy and childbirth, which, in the same way as eating on Pathogenia, has been systematically pathologised to the point where it barely feels reasonable or responsible to imagine it otherwise.
Pathogenesis
So what does that mean and why does it matter? A pathogenic approach to care focuses on identifying and treating illness. It assumes a mechanistic view of the body as a ‘faulty machine’1, generally using a limited range of physical morbidity, and mortality, as the sole measures of the success of the treatment. Iatrogenic harm, the range of potential harm caused by a treatment, is often disregarded, not given credence, or dismissed as a small price to pay. In pregnancy and childbirth, due largely to the fear of litigation, the bar for normality is set very low. The battery of tests and measures offered in pregnancy will on occasion pick up a serious health issue, but far more frequently it uncovers small ‘findings’ that are considered as being outside the range of normal even though the person remains well. The label ‘high risk’ is then applied to the now anxious mother, usually without any explanation that the actual increased risk for her or the baby is very small or even entirely uncertain, especially when weighed against the known risk of the treatment itself. She is then denied options known to increase safety and well-being such as home birth or birth in a midwife-led unit. Even those considered as ‘low risk’ are routinely hospitalised, and so profound and entrenched is the pathological mindset in regard to birth, few people think this odd. Yet, rather than improving outcomes for all, the hospital as a birth environment places a majority of healthy mothers at increased danger of experiencing a complex birth2, with 28,000 new mothers each year in the UK being diagnosed with post-traumatic stress disorder3, and many more going undiagnosed. Even when a birth is recorded as straightforward, if a person felt neglected, ignored, unbelieved, or unable to escape, and consequently in danger, it may have been experienced as trauma. Unfortunately, in a busy maternity unit, those feelings are experienced all too often.
Salutogenesis
In contrast, a salutogenic approach to health has a focus on the things that cause wellness. A term introduced through the work of Aaron Antonovsky4 salutogenesis comes from the Latin ‘salus’ meaning health and the Greek ‘genesis’ meaning origin or source. The primary sources of health include safety and security, good food and clean water, friendship and belonging, sound sleep, fresh clean air and exercise, pleasant surroundings, access to education, and good medical support within reach if and when needed. These are known as the social and physical determinants of health5. When they are in place, morbidity and mortality in all areas of health, including maternity, are very much reduced. Walking hand in hand with these external resources are qualities within the individual that also support and increase well-being. These include: self-determination, the belief that you have the right and ability to make your own decisions; self-efficacy6, the confidence that you have the ability to exert control over yourself and your environment in order to act on your decisions and accomplish your goal; and resilience, the ability to bounce back if the going has been tough and to remain hopeful and positive. In the salutogenic approach, wellness is not simply the absence of illness, but a far richer state that Aristotle referred to as Eudaimonia or human flourishing7. Salutogenesis underpins a holistic philosophy of care that does not separate different aspects of wellness, nor does it focus on one at the expense of another. Emotional, social and spiritual well-being are seen as not only inseparable from physical well-being, but as vital to it. The measure applied in the salutogenic approach to maternity care sets the bar high. It asks not simply that the mother and baby pull through, but that they and the new family flourish. However well-intentioned, routinely pathologising a normal physiological process by removing the healthy person from the very conditions that support wellness, and then undermining their autonomy, does not make sense. As expressed beautifully in the title of a newly published book by Lord Nigel Crisp, former Chief Executive of the NHS, ‘Health is Made at Home: Hospitals Are for Repairs’8.
A central tenet of salutogenic theory is ‘sense of coherence’9. The greater a person’s sense of coherence, the more able they are to navigate the normal stresses and uncertainties of life feeling healthy and resilient. A person with a strong sense of coherence views life as comprehensible, manageable, and meaningful. They understand or comprehend that life (including birth) is complex and uncertain, but they trust that with the resources available to them, they can manage inevitable challenges or conflicts in a way that is meaningful and satisfying. This leads to higher reported levels of well-being. On the other hand, a person with a low sense of coherence can more easily feel overwhelmed, out of control and unwell.
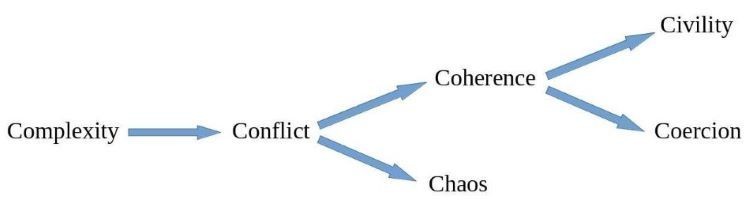
Antonovsky’s 6 Cs10 (p969)
Even when equipped with a strong sense of coherence, it is important that the individual is able to manage the challenge or conflict in an atmosphere of civility. This means that they should be able to express their needs and decisions in a calm and confident way, secure in the expectation that they will be listened to, believed, and their decisions respected. This maximises well-being for all concerned. When self-determination is met with coercive attempts to gain the person’s compliance, relationships of trust break down and the situation can become very stressful. Civility between health professionals also improves outcomes by creating a healthier and more civilised environment for everyone11, and this is helped when the physical environment is designed to support wellness12.
Maria is in her last month of pregnancy and, like almost all healthy women, is expecting to give birth in the warmth and familiarity of her own home. Naturally, she has been monitoring her own well-being supported by family and friends, but she also drops into the local maternity centre as often as she likes. While there she can enjoy a massage, chat with friends over lunch in the cafe, relax in the beautiful garden, join a walking or singing group, take a yoga or birth art class, find out about activities that are aimed for partners and families, or check in with her midwife. Each maternity centre is attended by the same small group of midwives, one of whom will be with Maria when she gives birth.
To ensure continuity of carer, each midwife is supported in their home life by a home-help. This is a vocational role often attracting people whose own children have grown. Home-helps are highly valued for the wisdom, compassion and skill they bring to supporting the well-being of the family. They also help care for people in labour, new families, the sick, the dying, and the newly bereaved as these natural life experiences often require a spare pair of experienced loving hands. They gain this experience through apprenticeship and are regarded as wise friends or aunties. When preferred, family members may assume this role and will be remunerated as fitting the importance of the work. Everyone acquires a solid grounding in these skills and philosophies at school, and from modelling within the home. Birth, death and illness are part of life, and life is everyone’s business. Health care on Salutogenia, including maternity care, is distinct from medical care. The government follows the paradigm, policy, practice approach. It has naturally adopted a salutogenic paradigm or philosophy of health, it has put policies in place known to support this, such as secure housing and minimising income inequality, and it has been conscientious in putting policy into practice. The result has been a massive improvement in well-being and a corresponding reduction in the costs of medicine. This has been possible because, as Antonovsky suspected13, people on Salutogenia care about each other.
Last week, Maria felt a bit odd and decided to drop in to see her midwife Sally. She was disappointed to find that a potential complication had arisen. However, she has grown up understanding that life is complex and challenges are inevitable. With her strong sense of coherence she rallies her resources. She contacts AIMS for evidence-based information and talks it through with her family. Then she checks in with Sally about the exact test readings and together they map out Maria’s different options. Maria knows that these are her decisions and hers alone, and that she will be supported whatever she decides.
As events unfold, Maria decides to have her baby in hospital. Women on Salutogenia tell wonderful stories about their hospital stays, not least about the food! The home birth culture, and the alternative of beautiful birth centres, have freed up the hospital system for those most needing medical care, thus improving outcomes and hugely reducing workplace stress. Combined with the deeply embedded culture of civility, reduced stress means that staff satisfaction, staff well-being and staff retention is optimised. The physical environment of the hospital is just gorgeous. With no extra demand on the budget, everything that is known about environmental psychology and well-being has been applied to the design of the building, furniture and decor, with measurable benefits for all within. Medical and clinical equipment is discreetly hidden but close to hand. The colours are warm and relaxing, the lighting can be adjusted, and nature is brought into each room in creative ways. People unable to access the hospital gardens for any reason can choose a nature-scape to be projected onto the walls and favourite music can be enjoyed. All of the factors that support physiological birth and perinatal transition are skilfully and lovingly applied to these more complex situations to great effect. Importantly, privacy, instinct and autonomy is respected at all times. Staff are encouraged and supported in this way of working because it fosters a matrix of trusting relationships that reduce trauma for parents and staff alike, and is cost effective in every way. Maria, like all new parents on Salutogenia, will come through the challenges of pregnancy and birth feeling safe, nurtured, respected and strong.

Birth room design informed by healing architecture and snoezelen theory14.
1 Davis-Floyd R. The technocratic, humanistic, and holistic paradigms of childbirth. International Journal of Gynecology & Obstetrics 75 (2001) S5-S23
2 NPEU (2012) The Birthplace cohort study: key findings. Nuffield department of Population Health. Available at: www.npeu.ox.ac.uk/birthplace/results (accessed: 21st January 2021)
3 Dekel S, Stuebe C, Dishy G. Childbirth Induced Posttraumatic Stress Syndrome: A Systematic Review of Prevalence and Risk Factors. Front Psychol. 2017;8:560. Published 2017 Apr 11. doi:10.3389/fpsyg.2017.00560
4 Antonovsky A, Sagy S. Aaron Antonovsky, the Scholar and the Man Behind Salutogenesis. 2016 Sep 3. In: Mittelmark MB, Sagy S, Eriksson M, et al., editors. The Handbook of Salutogenesis [Internet]. Cham (CH): Springer; 2017. Chapter 3. Available from: www.ncbi.nlm.nih.gov/books/NBK435855 doi: 10.1007/978-3-319-04600-6_3
5 Braveman P, Gottlieb L. The social determinants of health: it's time to consider the causes of the causes. Public Health Rep. 2014;129 Suppl 2(Suppl 2):19-31. doi:10.1177/00333549141291S206 (www.ncbi.nlm.nih.gov/pmc/articles/PMC3863696)
6 www.aims.org.uk/journal/item/self-efficacy-pregnancy-birth
7 Kraut, Richard, "Aristotle's Ethics", The Stanford Encyclopedia of Philosophy (Summer 2018 Edition), Edward N. Zalta (ed.), plato.stanford.edu/archives/sum2018/entries/aristotle-ethics.
8 Crisp N, (2020) Health is made at home, hospitals are for repairs : Building a healthy and health-creating society. United Kingdom. SALUS Global Knowledge Exchange.
9 Eriksson M. The Sense of Coherence in the Salutogenic Model of Health. 2016 Sep 3. In: Mittelmark MB, Sagy S, Eriksson M, et al., editors. The Handbook of Salutogenesis [Internet]. Cham (CH): Springer; 2017. Chapter 11. Available from: www.ncbi.nlm.nih.gov/books/NBK435812 doi: 10.1007/978-3-319-04600-6_11
10 Antonovsky, A. (1993a). Complexity, conflict, chaos, coherence, coercion and civility. Social Science & Medicine, 37(8), 969–981
11 Civility Saves Lives. Website. Available at: www.civilitysaveslives.com (accessed 28th January 2021)
12 Jenkinson, Bec & Josey, Natalie & Kruske, Sue. (2014). BirthSpace: An evidence-based guide to birth environment design.. 10.13140/RG.2.1.3962.8964.
13 Antonovsky, A. (1993b). Some salutogenic words of wisdom to the conferees. NHV, Göteborg. [Electronic] www.angelfire.com/ok/soc/agoteborg.html
14 Nielsen, J.H., Overgaard, C. Healing architecture and Snoezelen in delivery room design: a qualitative study of women’s birth experiences and patient-centeredness of care. BMC Pregnancy Childbirth 20, 283 (2020). https://doi.org/10.1186/s12884-020-02983-z
The AIMS Journal spearheads discussions about change and development in the maternity services.
AIMS Journal articles on the website go back to 1960, offering an important historical record of maternity issues over the past 60 years. Please check the date of the article because the situation that it discusses may have changed since it was published. We are also very aware that the language used in many articles may not be the language that AIMS would use today.
To contact the editors, please email: journal@aims.org.uk
We make the AIMS Journal freely available so that as many people as possible can benefit from the articles. If you found this article interesting please consider supporting us by becoming an AIMS member or making a donation. We are a small charity that accepts no commercial sponsorship, in order to preserve our reputation for providing impartial, evidence-based information.
AIMS supports all maternity service users to navigate the system as it exists, and campaigns for a system which truly meets the needs of all.